Every menopause journey is unique. We all bring our personal lived experiences, beliefs, family history, and heritage to this stage of life. And like other communities of color, there is great diversity among the Native Hawaiian and Pacific Islander peoples as well. However, all communities of color share something very important when it comes to health and well-being – an increased likelihood of experiencing health inequities and health situations that are more prominent in these communities. The menopause journey is a perfect time to take charge of your health and well-being. This “prescription for health” for Native Hawaiian and Pacific Islander women+ provides the information you need to live a healthier and perhaps longer life.
Native Hawaiian and Pacific Islander (NHPI) prescription for health
Ready to embrace well-being – before, during, or in post-menopause? It can help you manage symptoms and reduce the risk of certain conditions for which this natural stage of life puts you at increased risk.
Your prescription for health starts with understanding conditions for which you may be at higher risk because they disproportionately impact NHPI communities. These include:
- obesity
- cardiovascular disease
- diabetes
- mental health conditions (depression and anxiety)
- cancer
Although there are preventive steps you can take and guidance that may differ from one condition to another, there are certain things you can do to reduce your risk of developing a condition or managing it more effectively if you already have one. You can:
- Live a healthy lifestyle.
- Have a primary care practitioner who respects you, who listens, and whom you trust.
- Take the time to engage in preventive care services.
- Develop self-advocacy skills to help you get the care you need and deserve.
Let’s dive into each one so you’re aware of the signs for each condition and preventive steps you can take for improved health and well-being.
In the state of Hawaii, obesity had a prevalence of 40% of Native Hawaiians
and 44% of Pacific Islanders, according to data from the Hawaiʻi Health Data Warehouse.
Obesity
Despite what society tells us, obesity is understood to be a complex disease. It can increase the risk of and/or is accompanied by a broad spectrum of potential complications.
The list includes conditions like the following, just to name a few:
- Cardiovascular disease – hypertension, heart disease, stroke
- Diabetes
- High cholesterol
- GI reflux
- Gallbladder issues
- Sleep apnea
- Infertility
- Osteoarthritis from wear and tear on the joints
- Body pain
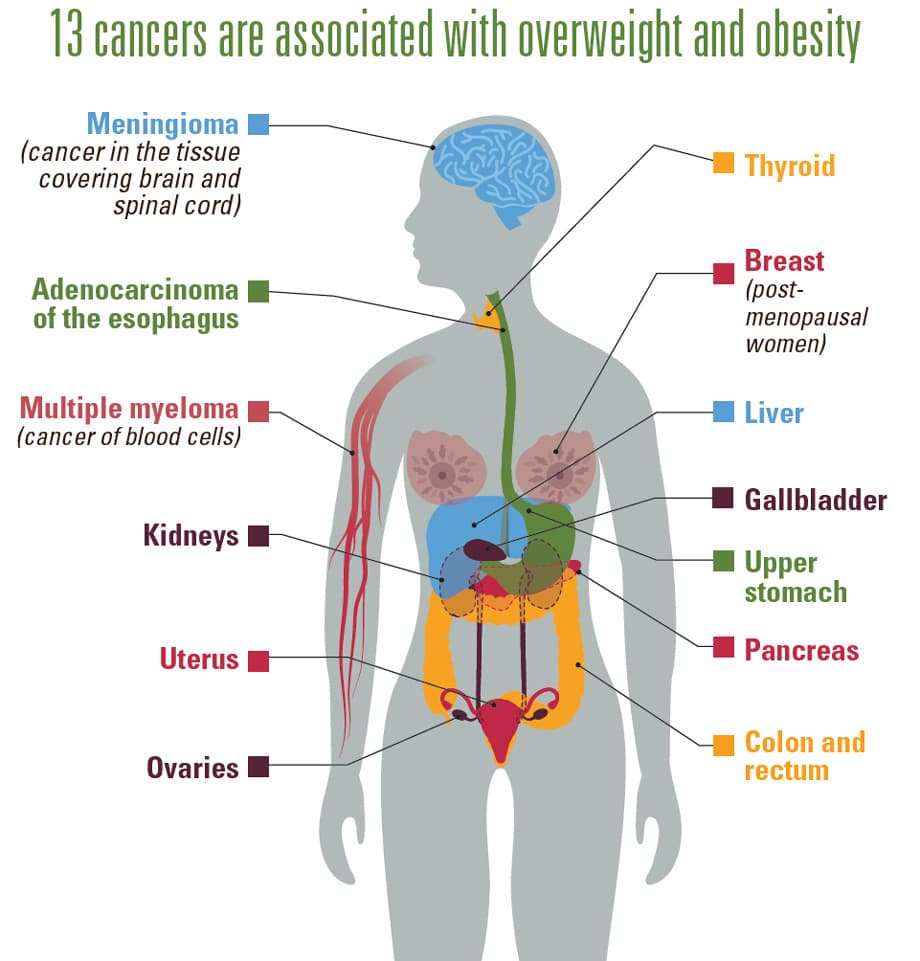
- Cancer
Those who are obese may also experience depression, anxiety, and low self-esteem.
The type of obesity where there is a lot of fat around the internal organs (vs. fat that’s just below the skin) is dangerous. It’s called visceral fat, and it sets up an inflammatory process that then leads or contributes to conditions like those above.
Body Mass Index (BMI) vs. waist circumference
Although body mass index (BMI) is the most commonly used way to categorize weight, it has become clear it disadvantages many groups (including communities of color and women) and may result in a person being deemed overweight/obese when they are not and vice versa.
One of the more common alternative ways to assess body fat is through a measure called waist circumference. If that number is above a certain number, then you would be considered obese and at risk for a multitude of conditions, as previously outlined.
In general, a female waist circumference should be less than 31.5 inches, and for males less than 37 inches.
Impact of diet
The change from a plant-based diet to a Western one contributes significantly with regard to the risk for obesity. The gut microbiome (collection of bacteria, viruses, and other microorganisms) is negatively impacted.
For example, studies of the Samoan population have found:
“the microbiomes of individuals change entirely in composition, shifting from predominantly Prevotella species (fiber-feeders) to Bacteroides species (associated with consumption of animal products).
When this shift occurs, there is a loss of the protective effects against weight gain that the plant-predominant diet had fostered in the microbiome.”
Additionally, an unhealthy gut microbiome (e.g., too many or too few organisms, an imbalance in the type of organisms, a lack of diversity) can impact certain hormones related to weight management:
Leptin
Controls the sensation of satiety (feeling full after eating); a low level of leptin due to an unhealthy gut microbiome would result in an increased appetite.
Ghrelin
Controls hunger; a high level of ghrelin due to an unhealthy gut microbiome would increase the sensation of hunger.
People who are obese can have leptin resistance and, therefore, don’t get the signal that they are full. And during perimenopause, ghrelin levels increase, which can lead to an increased feeling of hunger.
Stigma of obesity
Historically, obesity was viewed as a problem due to a lack of control/willpower or a character flaw. Things are changing, but not as fast as would be healthy for all concerned.
There is frequently still a stigma related to being overweight, particularly in parts of American society that put forth a beauty standard that often celebrates thinness, and often to an extreme extent.
Unfortunately, those with obesity can also experience bias and discrimination as a result of their weight.
During the menopause journey, food can be used as medicine to help you manage weight and symptoms. Try these foods for menopause.

NHPI communities are generally 2.5 times more likely to be diagnosed and die from diabetes than the white community,
and within the group, for Samoans the rate is even higher at 2.8 times, according to the Office of Minority Health.
Diabetes can be silent
Did you know you can be at risk for diabetes and not have any signs? This stage is called prediabetes. Your sugar (glucose) levels are higher than normal but not high enough for a diagnosis of diabetes.
You likely wouldn’t know you have this unless you have a blood test.
In fact, the CDC reports that even for those with a diagnosis of diabetes, 20% were not aware they had the condition.
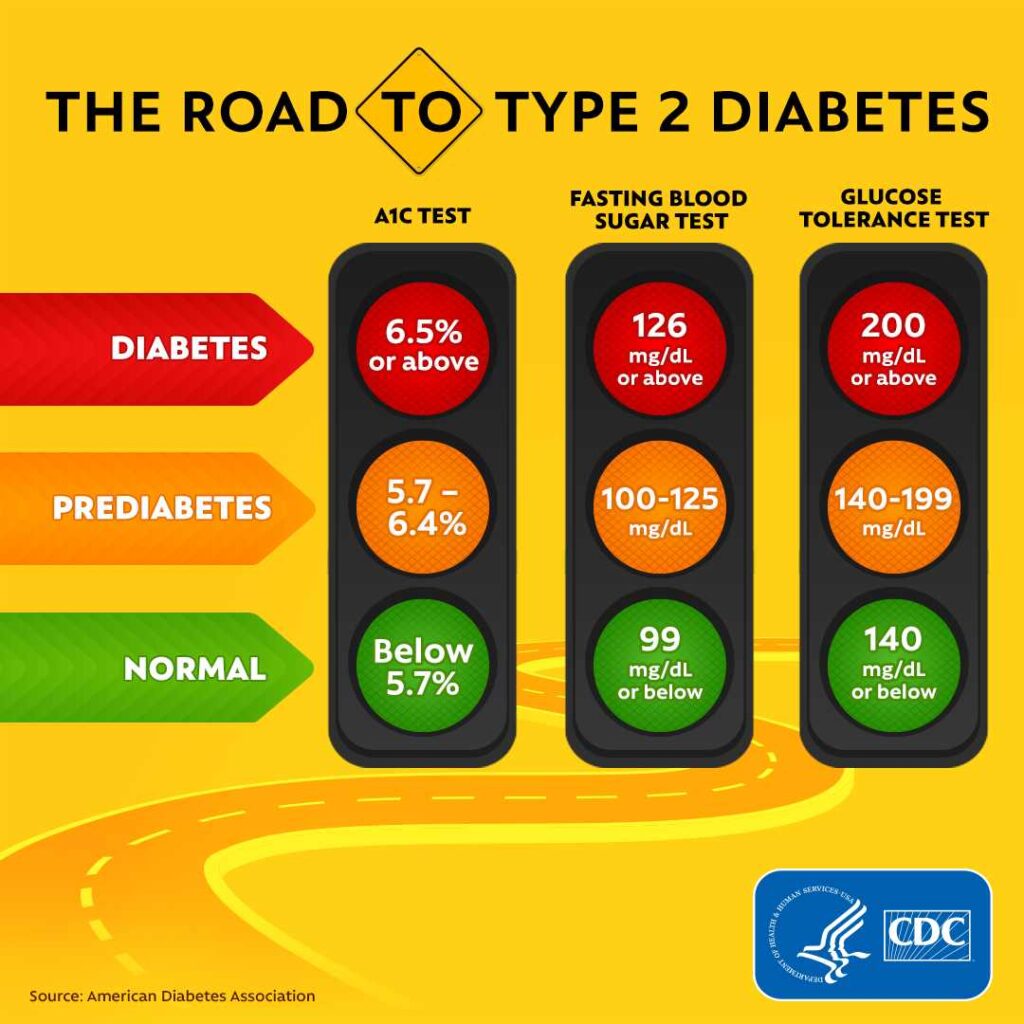
There are two types of diabetes:
Type 1
In type 1 diabetes, the body experiences an autoimmune process that stops the pancreas from secreting insulin. Insulin is used to take glucose into your cells to be used for energy and also to help the liver store blood sugar for future use.
An estimated 5 – 10% of those with diabetes have type 1.
Because no insulin is made, people with the condition need to take insulin daily (unless you are a candidate for a pancreatic islet cell transplantation).
Type 2
In type 2 diabetes, the body produces insulin but doesn’t use it effectively. As a result, it is difficult to keep blood sugar at normal levels.
Take an American Diabetes Association quiz to identify your potential risks.
Symptoms of Type 2 diabetes
For individuals with type 2 diabetes, symptoms may take a while to appear. When they do present, they include:
- Urinating more than usual
- Feeling very thirsty or hungry even after eating
- Feeling fatigued
- Blurred vision
- Having frequent infections or slow-healing cuts or sores (e.g., bottom of your feet, toes)
- Weight loss—even though you are eating more (type 1 diabetes)
- Having tingling, pain, or numbness in the hands or feet (type 2 diabetes)
Risk factors
Besides race/ethnicity, risk factors for diabetes include:
- First-degree relative with diabetes (type 2)
- Having a personal history of gestational (during pregnancy) diabetes or delivery of a baby who weighs 9 pounds or more
- Prediabetes
- Overweight/obesity with visceral fat (internal fat around the organs)
- Age 45 or older
- Being physically active less than 3 times a week
- Having fatty liver disease
- History of irregular periods or long menstrual cycle (40 days or more between periods)
Women+ are at greater risk of certain complications,
as well as depression associated with diabetes.
Diabetes complications for women+
Diabetes is the number one cause of adult blindness, kidney failure, and lower-limb amputations in the U.S. Diabetic women are at greater risk of developing those conditions.
Diabetes also increases the risk of heart disease (4 times more likely in women with diabetes), stroke, impaired hearing, and several cancers – breast, uterus, colon, liver, bladder and pancreas. And it’s the 8th leading cause of death.
Diabetes in women+ can also impact libido (decreases sexual desire), comfort and pleasure during penetrative sex (due to increased likelihood of vaginal dryness and decreased blood flow) and the likelihood of UTIs (increased).
All of these issues can also be seen as a result of genitourinary syndrome of menopause (GSM), with intensification of symptoms related to diabetes. Lastly, if you have diabetes during the menopause journey, you are more likely to have sleep issues, and they are more likely to be severe.
The hormonal fluctuations that occur during the menopause journey can lead to potentially increased challenges in managing blood sugar levels. Your periods may also involve heavier bleeding or last longer, and you may experience intensified food cravings.
As discussed earlier in the article, the NHPI community has a high rate of obesity. And combined with diabetes, the risk of cardiovascular disease is greater.
CVD is the most common causes of death in NHPI women.
Source: Centers for Disease Control National Center for Health Statistics
Cardiovascular disease (CVD)
During the menopause journey your risk for cardiovascular disease (CVD) increases due to the hormonal changes which occur. If you have experienced premature (age prior to 40) or early menopause (age greater than 40 but less than 45), your risk starts that much sooner and means it lasts for a greater number of years over the course of your lifetime.
Cardiovascular disease includes conditions like:
- hypertension
- heart disease
- stroke
- peripheral (in the limbs) artery disease (PAD)
The NHPI community has the second highest mortality rate due to CVD of all racial groups in the U.S. And NHPI people are more likely to suffer a stroke at a younger age.
Risk factors for the NHPI community
There are at least 18 risk factors for CVD. Besides obesity and diabetes, among those risk factors seen more commonly in the NHPI community are:
- Metabolic syndrome*
- High LDL (“bad” cholesterol)
- Hypertension (high blood pressure)
- Smoking
*Metabolic syndrome
Metabolic syndrome is diagnosed if a person has at least three of the following five conditions:
- excess internal body fat around your organs with a waist circumference ≥ 35 inches in women+ (≥ 31.5 inches if you are Asian)
- high blood sugar (glucose)
- high blood pressure
- a high blood triglyceride (a type of fat that can increase your LDL “bad” cholesterol) level
- low HDL cholesterol (“good” ) level
Symptoms for women+
It’s important to know that women+ may have different symptoms than the typical chest pain with radiation to the left arm and jaw when they are experiencing a heart attack.
Though things have improved over time, it is still the case that women+ seeking care in the ER may find their symptoms attributed to GI issues.
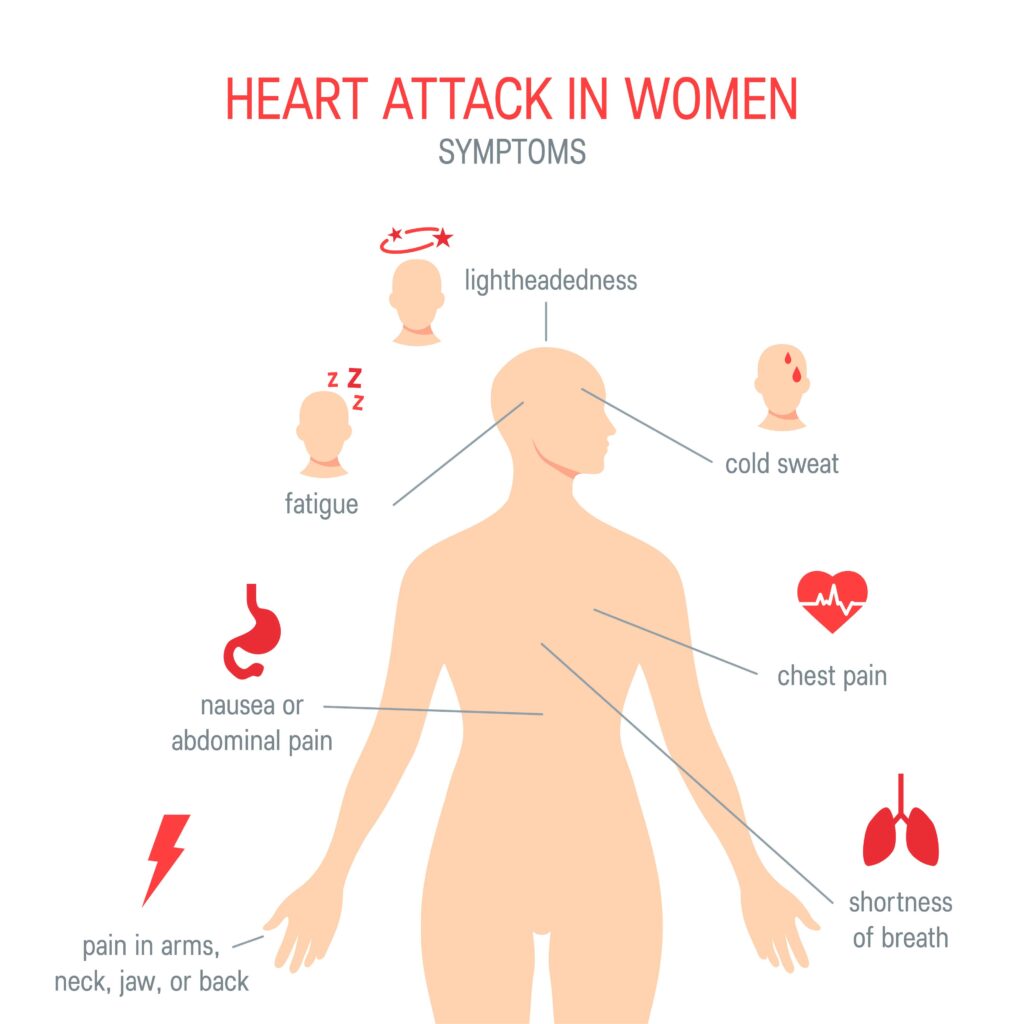
Studies also show women+ are also more likely to wait longer in the ER before being seen and not be treated according to clinical guidelines. They are also less likely to be evaluated with cardiac catheterization.
A treadmill stress test is usually the first way to evaluate for coronary artery disease in patients with symptoms. However, studies have shown a positive treadmill stress test is less accurate in women than men and should be followed up with additional testing, such as a stress echocardiogram.
As you can tell, it’s very important to be educated about signs and symptoms and to advocate for yourself to ensure you receive the most effective evaluation and treatment when heart disease is suspected!
Stroke symptoms
Stroke is a type of CVD. It’s important to know the symptoms of this condition as well. Getting treatment within a certain timeframe following the start of symptoms can make a significant difference as to whether or not you recover completely or are left with permanent changes, e.g., limited ability to walk or talk.
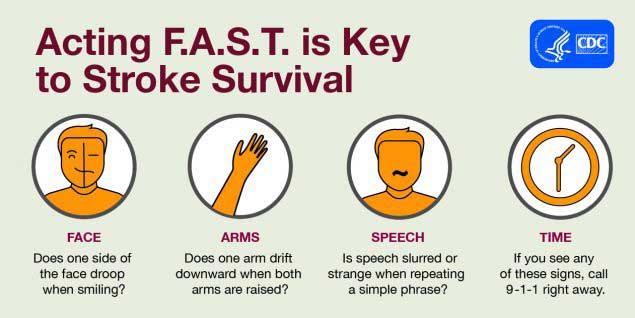
Learn more about hypertension and high cholesterol. Keeping your blood pressure under control and taking steps to maintain normal cholesterol are beneficial with regard to your risk of having a heart attack or stroke.
NHPI women had the largest number of cancer deaths overall from breast cancer.
Cancer
Unfortunately, in clinical research, when data collection is performed, NHPI people are often categorized with the Asian population even though they are very distinct groups. However, when the data is separated out, the conclusions that are made can be significant.
Native Hawaiian women have the highest incidence of cancer among NHPI ethnic groups. Compared with all other racial/ethnic groups, NHPI women had the highest death rates for:
- non-Hodgkin lymphoma (NHL)
- leukemia
- cancers of the cervix, uterus, oral cavity/pharynx, stomach, and soft tissue, including the heart
For example, when compared to the Asian community, studies have found NHPI women had the greatest rate of death related to cancer overall from breast cancer. They also had to wait a longer time beofre they were started on treatment and between each stage of therapy as well as a lower 10-year survival rate, according to a Stanford Medicine study.
And Native Hawaiian women diagnosed with a certain type of breast cancer (DCIS), which has a good prognosis and cure rate, are more likely to have a recurrence of a more invasive type of that cancer.
A lower survival rate has also been seen when it comes to uterine cancer.
Lifestyle habits to fight back against cancer
Although this information may be discouraging to learn, the good news is many factors that increase the risk of cancer and are seen commonly in NHPI women+ are also ones over which you have significant control. And taking action may also make some menopause symptoms less severe.
They include:
- physical inactivity
- unhealthy eating
- being overweight/obese
- smoking
- alcohol use
- too much sun exposure
- viral infection
Screening tests
For cancers like breast, cancer of the cervix, lung cancer, and colorectal cancer, there are screening tests available. And screening saves lives and makes it easier to catch things early!
Vaccinations to prevent viral cancers
In addition to screenings, vaccinations can help prevent against viral cancers.
Like the Asian community, NHPI people are more likely to develop cancers that can be related to infections, like liver (hepatitis B and C), stomach (Helicobacter pylori), and cervical (HPV).
To help reduce the chance of liver cancer caused by hepatitis B, there is a vaccination that is 80 – 100% effective to help prevent infection.
For hepatitis C, there is treatment (98% effective) that can eliminate the infection.
And if a Helicobacter pylori infection is found (the most common cause of stomach cancer), there is also treatment available that is 90-92% effective.
Be informed
Learn more from the American Cancer Society about the risk factors, screening tests, and treatments for the following cancers:

‘A’OHE PU’U KI’EKI’E KE HO’A’O ‘IA E PI’I
(No cliff is so tall it cannot be climbed.)
Mental health conditions
Mental health can be a concern at any time of life, but depression is especially a concern during perimenopause and the other stages of the journey. Know if you’re at risk and don’t be afraid to get help.
This is an important message for everyone, but especially in NHPI communities where there’s sometimes a reluctance.
Mental health stigmas for NHPI communities
We experienced a negative emotional health impact across the globe during the COVID-19 pandemic. And in many ways, we continue to feel its effects. However, the worldwide trauma has led to less stigma and taboo associated with mental health conditions and seeking help. But there is still much progress to be made.
A small study of Samoan and Marshallese people found a greater degree of stigma regarding mental health issues compared to the U.S. population as a whole.
A high percentage of participants attributed depression (73%) and schizophrenia (86%) to “either a person’s bad character or way they were raised.”
They were also more likely to believe mental health conditions would get better on their own and did not need treatment.
And a significant number of participants viewed those with mental health disorders to be dangerous and also had a reluctance to interact with them.
Know that these are stigmas only, and help is available.
NHPI mental health
During COVID, a needs assessment found 38% of NHPI survey participants reported having symptoms of anxiety or depression. The number was 50% in those who were Marshallese.
A survey by SAMHSA indicated that 15.7% of Native Hawaiian and Pacific Islanders reported having a substance use disorder.
Despite these numbers, NHPI adults are the racial group least likely to seek mental health services – 3 times less likely than their white counterparts. And unfortunately, when they do seek help, they are also 3 times less likely to receive mental health prescriptions and other mental health services. according to data from the Office of Minority Health.
Some of the reluctance may also be related to bias/discrimination/racism by healthcare providers resulting in a lower standard of care for the NHPI community.
Call 9-8-8

History and health disparities
Historically, Native Hawaiian and Pacific Islander communities naturally lived in a way that promoted health and sustainability of the land and other resources where people were geographically located. For example:
- a more plant-based eating pattern with lots of fruits and vegetables (for example the Waianae Diet)
- regular physical activity
- living in community to help maintain human connection and provide support to help cope with the challenges life might bring
The arrival of people from the West and occupation of lands which left natives displaced with expectations of acculturation [taking on the culture traits and habits of another (usually dominant) culture] resulted in a negative impact on the health, well-being, and longevity of the Native Hawaiian and Pacific Islander peoples which lasts to this day.
Besides the many deaths which resulted from exposure to infections not previously known to the population, there have been major shifts to:
- a lifestyle in which foods are often high in fat/sugar/salt
- exposure to environmental toxins and violence
- severe economic and educational disadvantages
Additionally, bias/discrimination/racism all contribute to a more challenging and stressful life, with a greater burden of chronic conditions and cancer that can result in premature death.
Factors that play a role in the development of health inequities are:
- health disparities
- social determinants of health (SDOH)
- the degree of health literacy a person has (not the same as general literacy)
- whether or not healthcare providers and systems have cultural sensitivity, humility, and competence
So, what does all that mean? Your health, well-being and longevity are impacted by things like:
- income and educational levels
- access to healthy food and water
- access to high-quality healthcare and insurance
- being respected and believed when you seek care
- exposure to trauma or bias/discrimination/racism/genderism/anti-LGBTQIA+ hate
For example, you may be at greater risk for certain cancers or chronic conditions, be more likely to experience medical gaslighting, or have a delayed diagnosis.
The impact can be even more significant and extend through the generation if you are older, have a disability, live in a rural vs. urban setting or in particular parts of the country, are in the gender identity or sexual orientation minority, are an immigrant vs. born in the country or have language barriers, or have been dispossessed from your native land.
It also means your menopause journey as a woman+ of color (or as a person at the intersection of gender identity and sexual orientation) may be different compared to other racial groups as well as between ethnicities within a racial group.

Hibiscus (state flower of Hawaii) and Sea Turtle (symbol of strength and longevity)
You have the power
More than ever, at this stage of your life, you have everything to gain both now and for the years ahead by taking good care of yourself – body, mind, and spirit.
There are at least 4 fantastic reasons to be motivated to do so:
- potential to reduce the severity of menopausal symptoms
- decreasing your risk of physical and mental health chronic conditions, which are more likely to develop during the menopause journey due to the hormonal changes that occur
- increasing your chances of having a greater quality of life for a longer period of time
- potentially increasing your lifespan
Value of social connection
Having human connection and a strong social network is among the factors found in “Blue Zones,” parts of the world where people live longer and healthier lives; instead of living to 80, people live to 100 in Blue Zone regions around the world without chronic disease.
In NHPI communities, studies have found that high perceived social cohesion is beneficial when it comes to engaging in physical activity, managing obesity, seeking preventive care services, getting good quality sleep, and mental health issues.
According to Healthy People 2030, social cohesion is
“the strength of relationships and the sense of solidarity among members of a community.”
Make positive changes
Take the time to live a healthy lifestyle, and find new ways to manage. Small steps can make a big difference in how you feel and in your menopausal symptoms. Focus on:
- healthy eating
- physical activity
- sleep hygiene
- self-care to de-stress and form coping strategies
- stay up-to-date and vigilant about preventive care develop the advocacy skills to get the care you need and deserve
- find a healthcare practitioner with expertise in menopause management
You have the power to make a change for the better! You also have the opportunity to make this stage of life a positive and transformative start to great things ahead!
Resources
Free Support
For A Limited Time!
pausitive health offers personalized support for every stage of the menopause journey. Customize your experience with 14 evidence-based educational tracks, a diet assessment with recommendations and a food library, solutions for aches and pains, virtual care options, practical lifestyle supports, and a supportive community. All in one trusted place.
Join the pilot and be the first to know when our web-app is coming in 2026!
Health inequities and their causes | World Health Organization
Home | Navigating Your Healthcare Journey
Overweight and Obesity | Hawai’i Health Data Warehouse
Neuendorf S, Neuendorf J, Yakub M. Origin, Impact, and Solutions for Lifestyle-Related Chronic Diseases in Samoa and American Samoa. Cureus. 2021 Sep 5;13(9):e17749. doi: 10.7759/cureus.17749. PMID: 34659962; PMCID: PMC8493186.
van Son J, Koekkoek LL, La Fleur SE, Serlie MJ, Nieuwdorp M. The Role of the Gut Microbiota in the Gut–Brain Axis in Obesity: Mechanisms and Future Implications. International Journal of Molecular Sciences. 2021; 22(6):2993. https://doi.org/10.3390/ijms22062993
Sowers MR, Wildman RP, Mancuso P, Eyvazzadeh AD, Karvonen-Gutierrez CA, Rillamas-Sun E, Jannausch ML. Change in adipocytokines and ghrelin with menopause. Maturitas. 2008 Feb 20;59(2):149-57. doi: 10.1016/j.maturitas.2007.12.006. Epub 2008 Feb 14. PMID: 18280066; PMCID: PMC2311418.
Elflein J. Prevalence of diagnosed diabetes among adults aged 18 and over in the U.S. from 2000 to 2022. Statista. Feb 6, 2024
Diabetes and Native Hawaiians/Pacific Islanders | Office of Minority Health
Diabetes and Women | Centers for Disease Control and Prevention
Diabetes Tests | Centers for Disease Control and Prevention
Diabetes Fast Facts | Centers for Disease Control and Prevention
The Road To Type 2 Diabetes Infographic | Centers for Disease Control and Prevention
Take the Type 2 Risk Test | American Diabetes Association
Diabetes and Heart Disease | Johns Hopkins Medicine
Diabetes and Hearing Loss | Centers for Disease Control and Prevention
Giovannucci E, Harlan DM, Archer MC, Bergenstal RM, Gapstur SM, Habel LA, Pollak M, Regensteiner JG, Yee D. Diabetes and cancer: a consensus report. Diabetes Care. 2010 Jul;33(7):1674-85. doi: 10.2337/dc10-0666. PMID: 20587728; PMCID: PMC2890380.
Wang Y, Shan Z, Arvizu M, et al. Associations of Menstrual Cycle Characteristics Across the Reproductive Life Span and Lifestyle Factors With Risk of Type 2 Diabetes. JAMA Netw Open. 2020;3(12):e2027928. doi:10.1001/jamanetworkopen.2020.27928
Im, Eun-Ok PhD, MPH, FAAN; Yang, You Lee PhD, RN; Liu, Jianghong PhD, RN, FAAN; Chee, Wonshik PhD. Sleep-related symptoms of midlife women with and without type 2 diabetes mellitus. Menopause 26(10):p 1178-1184, October 2019. | DOI: 10.1097/GME.0000000000001383
Health of Native Hawaiian or Other Pacific Islander non-Hispanic POpulation | Centers for Disease Control and Prevention
Woodruff R, Kaholokula J, Riley L, Loustalot F, Vaughan A, Diktonaite K, Richardson L, Tong X. Cardiovascular Disease Mortality Trends Among Native Hawaiian and Pacific Islander Adults—United States, 2018 to 2022. Circulation. 2023; 148:A12190. https://doi.org/10.1161/circ.148.suppl_1.12190
Nakagawa K, Koenig MA, Asai SM, Chang CW, Seto TB. Disparities among Asians and native Hawaiians and Pacific Islanders with ischemic stroke. Neurology. 2013 Feb 26;80(9):839-43. doi: 10.1212/WNL.0b013e3182840797. Epub 2013 Jan 30. PMID: 23365055; PMCID: PMC3598459.
Stroke and Native Hawaiians/Pacific Islanders | Office of Minority Health
AHA Scientific Statement. Acute Myocardial Infarction in Women. Circulation. 2016 | Volume 133, Issue 9: 916–947, January 25, 2016, https://doi.org/10.1161/CIR.0000000000000351
Chamsi-Pasha MA, Kurrelmeyer KM. Noninvasive Evaluation of Symptomatic Women with Suspected Coronary Artery Disease. Methodist Debakey Cardiovasc J. 2017 Oct-Dec;13(4):193-200. doi: 10.14797/mdcj-13-4-193. PMID: 29744011; PMCID: PMC5935278.
Acting F.A.S.T. is Key to Stroke Survival Infographic | Centers for Disease Control and Prevention
High Blood Pressure | Centers for Disease Control and Prevention
Cholesterol | Centers for Disease Control and Prevention
Breast Cancer: Pharmacologic Management | Cancer Therapy Advisor
Hodgkin Lymphoma: Pharmacologic Treatment | Cancer Therapy Advisor
13 Cancers Are Associated with Overweight and Obesity Infographic | Centers for Disease Control and Prevention
Cancer Death Rates Higher in NHPI Patients Than in Asian Patients | Cancer Therapy Advisor
Breast cancer disparities in Native Hawaiians and Pacific Islanders masked in larger ‘Asian American’ group |
Stanford Medicine
Taparra K, Qu V, Pollom E. Disparities in Survival and Comorbidity Burden Between Asian and Native Hawaiian and Other Pacific Islander Patients With Cancer. JAMA Netw Open. 2022;5(8):e2226327. doi:10.1001/jamanetworkopen.2022.26327
Taparra K, Fukui J, Killeen J, Sumida K, Loo LWM, Hernandez BY. Racial and Ethnic Disparities in Rates of Invasive Second Breast Cancer Among Women With Ductal Carcinoma In Situ in Hawai’i. JAMA Netw Open. 2021 Oct 1;4(10):e2128977. doi: 10.1001/jamanetworkopen.2021.28977. PMID: 34668945; PMCID: PMC8529402.
Taparra K et. al. Navigating Native Hawaiian and Pacific Islander Cancer Disparities From a Cultural and Historical Perspective. JCO Oncology Practice. Volume 17, Number 3 https://doi.org/10.1200/OP.20.00831
Haque A, Berrington de González A, Chen Y, Haozous E, Inoue-Choi M, Lawrence W, McGee-Avila J, Nápoles A, Pérez-Stable E, Taparra K, Vo J, Freedman N, Shiels M. Cancer mortality rates by racial and ethnic groups in the United States, 2018-2020. JNCI: Journal of the National Cancer Institute, Volume 115, Issue 7, July 2023, Pages 822–830, https://doi.org/10.1093/jnci/djad069
Hepatitis B | U.S. Department of Health and Human Services
Manns, M.P., Maasoumy, B. Breakthroughs in hepatitis C research: from discovery to cure. Nat Rev Gastroenterol Hepatol 19, 533–550 (2022). https://doi.org/10.1038/s41575-022-00608-8
Jonaitis P, Kupcinskas J, Nyssen OP, Puig I, Gisbert JP, Jonaitis L. Evaluation of the Effectiveness of Helicobacter pylori Eradication Regimens in Lithuania during the Years 2013-2020: Data from the European Registry on Helicobacter pylori Management (Hp-EuReg). Medicina (Kaunas). 2021 Jun 23;57(7):642. doi: 10.3390/medicina57070642. PMID: 34201428; PMCID: PMC8305910.
Home, Breast, Cervical, Colorectal, Liver, Lung, Ovarian, Skin, Stomach, Uterine | American Cancer Society
Native Hawaiian/Pacific Islander COVID-19 Needs Assessment Executive Summary | AAPA
2021 NSDUH Annual National Report | Substance Abuse and Mental Health Services Administration
Mental and Behavioral Health – Native Hawaiians/Pacific Islanders | Office of Minority Health
Racism and Health [YouTube] | Centers for Disease Control and Prevention
Subica AM, Aitaoto N, Sullivan JG, Henwood BF, Yamada AM, Link BG. Mental illness stigma among Pacific Islanders. Psychiatry Res. 2019 Mar;273:578-585. doi: 10.1016/j.psychres.2019.01.077. Epub 2019 Jan 26. PMID: 30716597; PMCID: PMC6561790.
2018 National Survey on Drug Use and Health: Asians/Native Hawaiians and Other Pacific Islanders (NHOPI) | Substance Abuse and Mental Health Services Administration
988 | National Suicide & Crisis Lifeline
Hawaii album, p. 14, Honolulu scenes and landscapes | Library of Congress
1991: Waianae Diet promotes Native Hawaiian culture, well-being | Native Voices – National Library of Medicine
Wang ML, Narcisse M-R, Alatorre S, Kozak AT, McElfish PA. Neighborhood social cohesion and physical activity and obesity outcomes among Native Hawaiian and Pacific Islander individuals. Obesity (Silver Spring). 2022; 30: 249–256. doi:10.1002/oby.23298
Young M, Gerber M, Ash T, Horan C, Taveras E. Neighborhood social cohesion and sleep outcomes in the Native Hawaiian and Pacific Islander National Health Interview Survey. Sleep, Volume 41, Issue 9, September 2018, zsy097, https://doi.org/10.1093/sleep/zsy097
Lee YJ, Braun KL, Wu YY, Hong S, Gonzales E, Wang Y, Hossain MD, Terada TM, Browne CV. Neighborhood Social Cohesion and the Health of Native Hawaiian and Other Pacific Islander Older Adults. J Gerontol Soc Work. 2022 Jan;65(1):3-23. doi: 10.1080/01634372.2021.1917033. Epub 2021 May 11. PMID: 33974515.
Healthy People 2030 | U.S. Department of Health and Human Services
Heart Matters – Why Your Waist Size Matters | British Heart Foundation
Home | American Diabetes Association
Asian Americans/Pacific Islanders | Anxiety & Depression Association of America
AANHPI Service Providers in All Fifty States | National Asian American Pacific Islander Mental Health Association
Take a Mental Health Test | Mental Health America
Home | Crisis Text Line
You may also like…

18 Cardiovascular Risk Factors Menopausal Women Need To Know
Cardiovascular disease (CVD) is the #1 killer in women. Learn 18 cardiovascular risk factors menopausal women need to know.

Foods For Menopause: 9 Best Foods To Help Menopause
Did you know you can manage your menopause symptoms with food? Learn the 10 best foods packed with the necessary nutrients to feel better.

Menopause Exercise Videos To Improve How You Feel
Try these menopause exercise videos to improve how you feel. They can help with weight loss, body strength, and flexibility.